Air purification in hospitals is a critical aspect of infection control and patient safety, evolving alongside advancements in healthcare and a growing understanding of airborne disease transmission. The need for sophisticated air purification systems has never been greater, driven by factors like increasing antibiotic resistance, the emergence of new pathogens, and a larger population of immunocompromised individuals. Effective air purifier used in hospitals contribute to a healthier environment for patients, staff, and visitors, reducing the risk of healthcare-associated infections (HAIs).
Globally, hospitals are facing increasing pressure to maintain air quality standards that meet or exceed stringent regulatory guidelines. This demand is particularly acute in densely populated urban areas and regions with high levels of air pollution. The cost of HAIs is substantial, encompassing extended hospital stays, increased treatment expenses, and potentially life-threatening complications. Investing in advanced air purifier used in hospitals is, therefore, not merely a matter of compliance but a vital component of responsible healthcare management.
The selection and implementation of appropriate air purification technologies require careful consideration of factors such as filtration efficiency, air exchange rates, noise levels, and energy consumption. Modern hospitals are increasingly adopting integrated air management systems that combine filtration with ventilation and monitoring capabilities to create a comprehensive approach to indoor air quality control.

Maintaining optimal air quality within hospital environments is paramount for patient recovery and preventing the spread of infections. Hospitals are inherently vulnerable to airborne pathogens, and patients, especially those with compromised immune systems, are particularly susceptible. Effective air purifier used in hospitals plays a crucial role in mitigating these risks, ensuring a safer and more hygienic healthcare environment.
The presence of airborne contaminants, including bacteria, viruses, fungi, and particulate matter, can exacerbate respiratory conditions and hinder the healing process. Therefore, comprehensive air purification strategies are essential for creating a protective barrier against these threats, contributing to improved patient outcomes and reduced healthcare costs.
An air purifier used in hospitals is a device designed to remove contaminants from the air, typically employing filtration, sterilization, or a combination of both. Unlike standard residential air purifiers, hospital-grade systems are engineered to meet rigorous performance standards and address the specific challenges of a healthcare environment. These systems are designed to capture a wide range of airborne particles, including bacteria, viruses, fungal spores, dust, pollen, and volatile organic compounds (VOCs).
The core function of these devices is to reduce the concentration of harmful airborne pathogens and pollutants, creating a cleaner and safer atmosphere for patients, staff, and visitors. They are essential in areas such as operating rooms, intensive care units (ICUs), isolation wards, and waiting rooms, where the risk of infection is particularly high.
Modern air purifier used in hospitals often incorporate advanced technologies such as HEPA filters, activated carbon filters, and UV-C sterilization to achieve superior air quality and infection control.
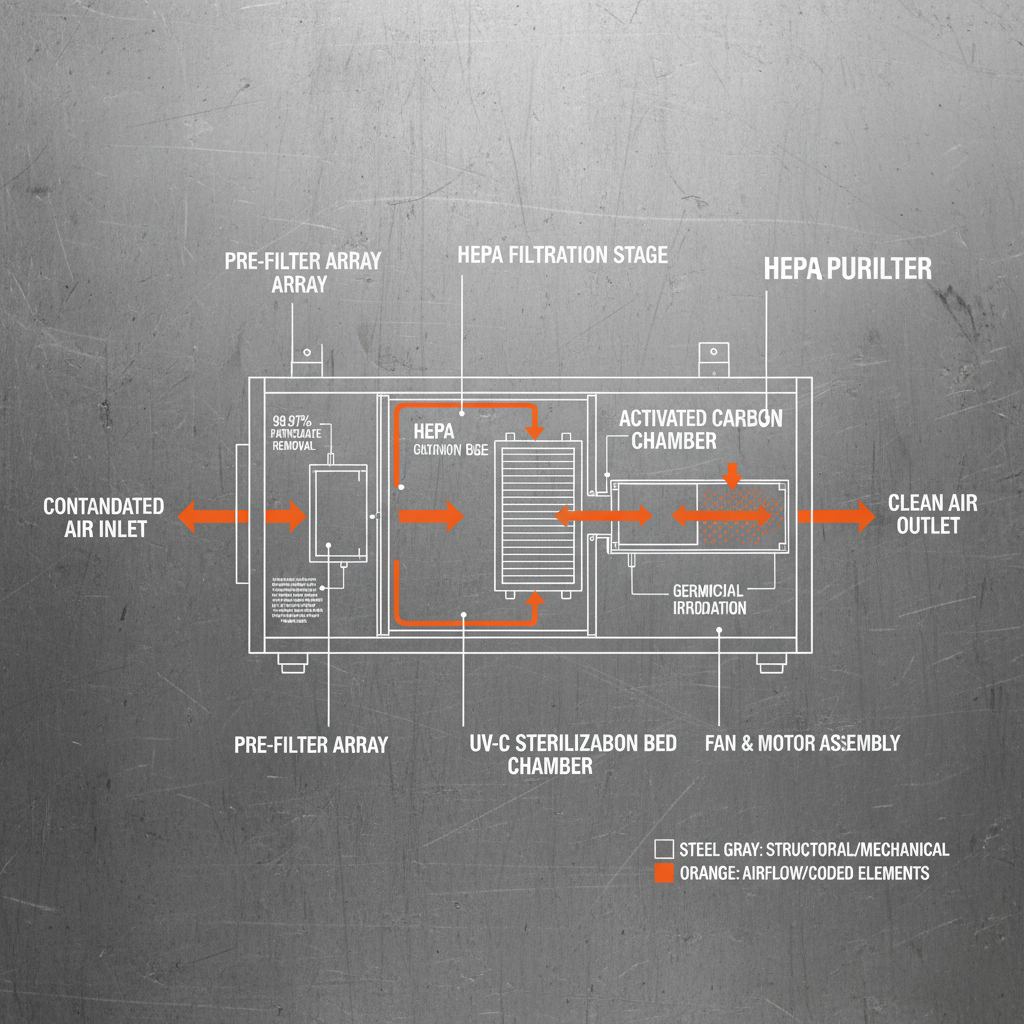
Hospital air purification systems comprise several key components working in concert to deliver effective air cleaning. One crucial element is the pre-filter, which captures larger particles like dust and pollen, extending the lifespan of subsequent filters. Following the pre-filter is often a HEPA (High-Efficiency Particulate Air) filter, capable of removing at least 99.97% of particles 0.3 microns in diameter, including bacteria and viruses.
Activated carbon filters are also frequently incorporated to absorb odors, gases, and VOCs, contributing to improved air quality and patient comfort. Many systems include UV-C lamps, which utilize ultraviolet light to neutralize airborne pathogens by disrupting their DNA. Finally, the system’s fan and airflow design are critical for ensuring adequate air circulation and maximizing filter efficiency.
The integration of these components, combined with regular maintenance and filter replacement, is essential for maintaining the effectiveness of the air purification system and safeguarding against airborne contamination within the hospital environment.
Several factors can significantly influence the performance of air purifier used in hospitals. Air change rate (ACH), which represents the number of times the air in a room is completely replaced per hour, is a critical metric. Higher ACH values indicate more frequent air exchange and more effective purification. Room size and layout also play a role, as larger spaces require more powerful systems to achieve adequate air circulation.
Filter quality is paramount; HEPA filters must meet stringent standards to ensure effective particle removal. Proper filter maintenance, including regular replacement according to manufacturer’s guidelines, is crucial for maintaining optimal performance. Additionally, airflow patterns and the placement of air purification units can impact their effectiveness, requiring careful consideration during system design and installation.
Air purifier used in hospitals are deployed in a wide range of healthcare settings worldwide. Operating rooms require the highest level of air purification to minimize the risk of surgical site infections. Intensive care units (ICUs), where critically ill patients are more vulnerable to airborne pathogens, also rely heavily on these systems.
Isolation wards, used to contain patients with infectious diseases, benefit significantly from dedicated air purification units to prevent cross-contamination. Emergency departments, with their high patient turnover and potential for exposure to various pathogens, also require robust air purification measures. Hospitals in regions with high levels of air pollution, such as major urban centers in Asia and Latin America, are particularly reliant on advanced air purification technologies.
The advantages of implementing effective air purification systems in hospitals extend beyond infection control. Reduced HAIs translate to shorter hospital stays, lower treatment costs, and improved patient satisfaction. Enhanced air quality can also benefit hospital staff, reducing their exposure to airborne pathogens and improving their overall health and well-being.
Investing in air purifier used in hospitals demonstrates a commitment to patient safety and quality care, enhancing the hospital’s reputation and building trust with the community. Long-term cost savings associated with reduced infection rates and improved operational efficiency further contribute to the value proposition.
These systems contribute to a more sustainable healthcare environment by minimizing the need for aggressive antimicrobial treatments and reducing the overall burden of infectious diseases.
The field of hospital air purification is constantly evolving, with ongoing research and development focused on improving efficiency, reducing energy consumption, and enhancing pathogen removal capabilities. Smart air purification systems, integrated with building management systems and real-time air quality monitoring sensors, are gaining traction. These systems can automatically adjust filtration levels based on occupancy and air quality data, optimizing performance and minimizing energy waste.
Nanotechnology-based filters, capable of capturing even smaller particles, are also under development. Furthermore, advancements in UV-C sterilization technology, including the use of pulsed UV-C lamps and photocatalytic oxidation (PCO) systems, promise to deliver more effective and energy-efficient disinfection solutions.
The integration of artificial intelligence (AI) and machine learning (ML) algorithms into air purification systems will enable predictive maintenance, optimized filter replacement schedules, and improved overall system performance.
| Challenge | Impact on Air Quality | Potential Solution | Implementation Complexity |
|---|---|---|---|
| High Initial Cost | May limit adoption in resource-constrained hospitals | Lease programs, government subsidies, long-term cost analysis | Medium |
| Filter Maintenance & Replacement | Reduced efficiency, potential for pathogen release | Automated filter monitoring, scheduled maintenance contracts | Low |
| Noise Levels | Patient and staff discomfort | Selection of low-noise units, strategic placement | Low |
| Energy Consumption | Increased operating costs, environmental impact | Energy-efficient filters, variable speed fans, smart controls | Medium |
| Airflow Disruption | Compromised ventilation effectiveness | Proper system design, integration with HVAC systems | High |
| Lack of Real-time Monitoring | Delayed response to air quality changes | Integration with air quality sensors and data analytics | Medium |
HEPA filters are far more effective than standard air filters. HEPA (High-Efficiency Particulate Air) filters are designed to capture at least 99.97% of particles 0.3 microns in diameter, including bacteria, viruses, and fungal spores. Standard air filters, while capturing larger particles like dust and pollen, lack the fine filtration capabilities required for hospital-grade air purification, making them unsuitable for infection control.
Filter replacement frequency depends on the type of filter, the air quality in the hospital, and the unit’s usage. Pre-filters typically need to be replaced monthly, while HEPA filters may last 6-12 months. Activated carbon filters often require replacement every 3-6 months. Regular monitoring and adherence to the manufacturer’s recommendations are crucial for maintaining optimal performance and preventing reduced filtration efficiency.
UV-C lights can be effective in neutralizing airborne pathogens by disrupting their DNA, rendering them harmless. However, UV-C effectiveness relies on adequate exposure time and intensity. It's essential that the UV-C light source is shielded to prevent direct exposure to humans. UV-C is often used in combination with filtration for a more comprehensive air purification solution.
The recommended ACH varies depending on the specific hospital area. Operating rooms and ICUs typically require higher ACH (6-12 or more) than general patient rooms (4-6). Isolation rooms for airborne infectious diseases may necessitate even higher ACH rates. Adhering to ASHRAE standards and local regulations is crucial for determining appropriate ACH levels.
Regular maintenance, including filter replacements, system inspections, and airflow measurements, is essential. Consider implementing a preventive maintenance schedule and training staff on proper operation and troubleshooting. Periodic air quality testing can verify system performance and identify potential issues. Partnering with a qualified HVAC professional specializing in hospital air purification is highly recommended.
The cost varies greatly based on the size of the hospital, the number of rooms needing purification, the type of system chosen (portable units vs. integrated systems), and ongoing maintenance expenses. Initial costs can range from a few thousand to hundreds of thousands of dollars. However, the long-term benefits, including reduced infection rates and improved patient outcomes, often outweigh the initial investment.
In conclusion, air purifier used in hospitals are essential components of modern healthcare facilities, playing a vital role in protecting patients, staff, and visitors from airborne pathogens and pollutants. Investing in advanced air purification technologies is not merely a matter of compliance but a critical step towards enhancing patient safety, improving outcomes, and creating a healthier healthcare environment. Proper selection, implementation, and maintenance of these systems are paramount to realizing their full potential.
Looking ahead, continued innovation in air purification technologies, coupled with the integration of smart systems and real-time monitoring, will further enhance their effectiveness and efficiency. Healthcare facilities should prioritize air quality as a core element of their infection control strategies, recognizing the significant impact it has on overall patient well-being and the long-term sustainability of healthcare operations. Visit our website at www.meshmachinery.com to learn more about our hospital-grade air purification solutions.